Real-Time Tracking for Patient Mentorship Programs
Key Takeaways
Real-time tracking is changing how patient mentorship programs work by replacing outdated methods with digital tools that centralize communication, monitor interactions, and provide instant insights. These platforms prioritize privacy, use smart algorithms to match patients with suitable mentors, and offer data-driven solutions to improve outcomes. Key features include:
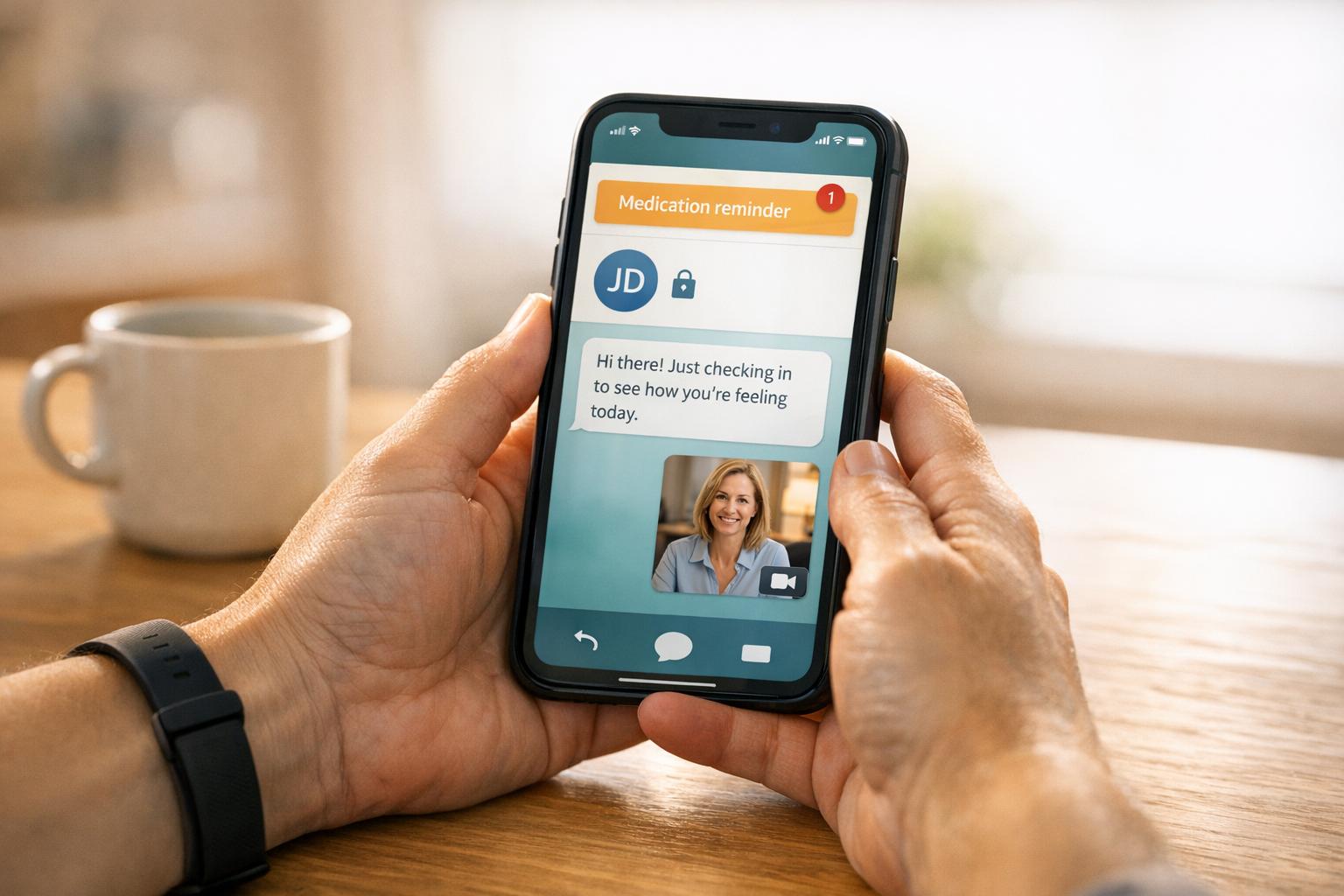
- Secure Communication: Tools like PatientPartner ensure private, in-platform interactions, protecting personal details.
- Real-Time Alerts: Notify care teams about critical moments, such as patient hesitation or engagement drops.
- Personalization: Matches patients with mentors based on shared experiences, medical conditions, or location.
- Outcome Tracking: Measures metrics like therapy adherence, patient confidence, and treatment adoption rates.
From dashboards like PatientPartner to telehealth tools for recovery programs and diabetes mentoring, these systems boost patient support with real-time data and tailored care. However, challenges like data privacy, regulatory hurdles, and potential monitoring fatigue need careful management to maintain patient trust and program efficiency.
1. PatientPartner Real-Time Dashboard
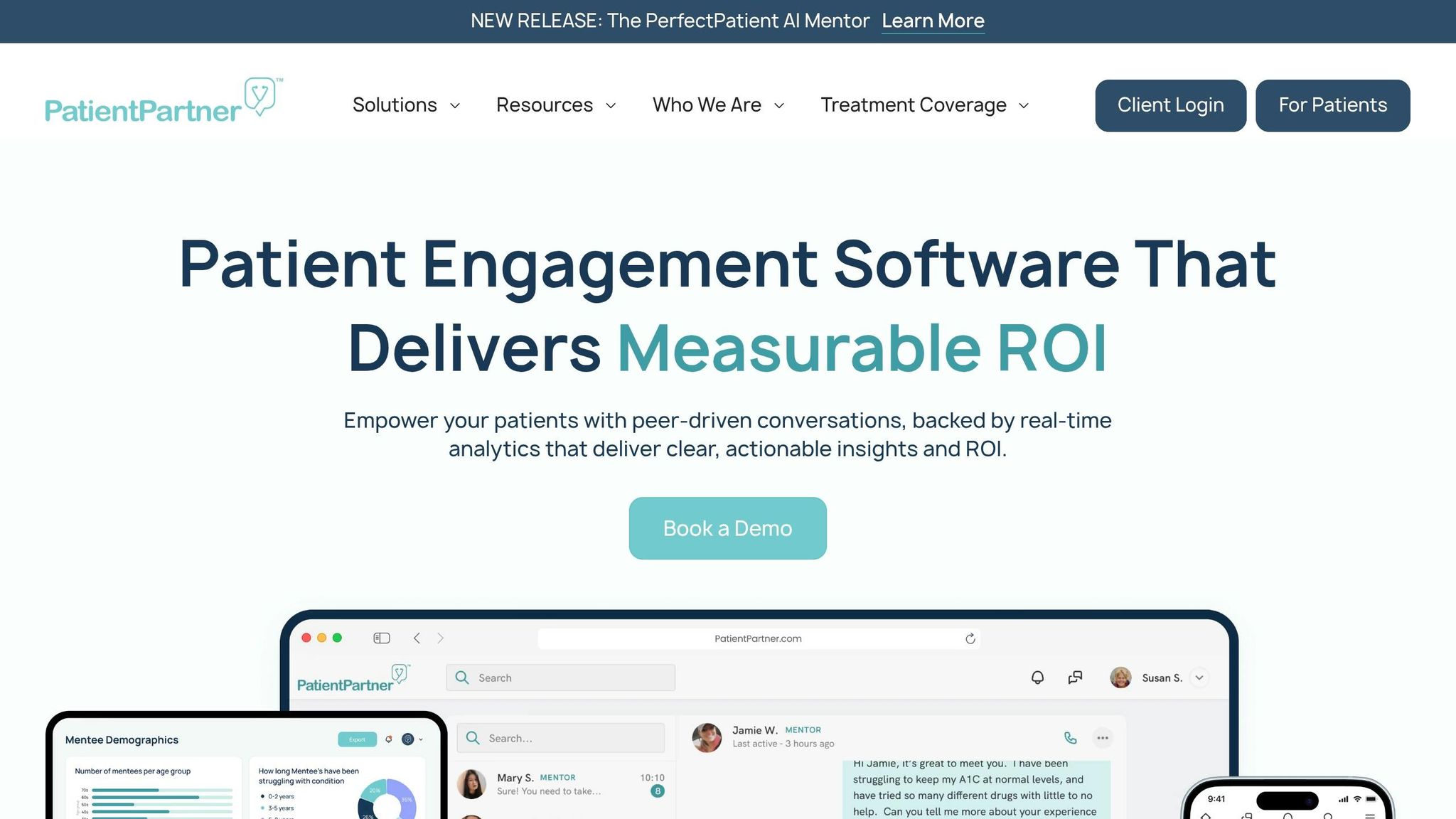
The PatientPartner Real-Time Dashboard brings mentor–patient interactions into one centralized platform. While traditional analytics rely on historical data, this dashboard delivers instant insights into engagement levels, patient feelings, and program results. This immediate access empowers quicker decisions and proactive actions, laying the groundwork for the detailed features outlined below.
Real-Time Alerts
With automated alerts, the dashboard keeps patient service teams informed about key events, such as when a mentor–patient conversation reaches a pivotal point or when sentiment analysis flags potential treatment adoption challenges. Importantly, the system avoids overloading users with unnecessary notifications. Studies highlight that excessive alerting can lead to "alert fatigue", where critical updates are overlooked. PatientPartner combats this by reserving high-priority alerts for moments that truly demand attention, like a patient expressing hesitation about starting treatment or a sudden drop in engagement.
Data Accuracy
The platform ensures reliable data by integrating directly with existing systems and capturing information in real time from mentor–patient interactions. This accuracy supports informed, proactive decisions. For instance, a healthcare provider in Washington leveraged real-time data and AI tools to cut "lost cases" by 20% within six months. This example underscores how precise, immediate data can significantly improve patient outcomes.
Personalization
The dashboard offers customizable reports tailored to the needs of different teams within pharmaceutical and med-tech organizations. Marketing teams can monitor engagement and new patient start metrics, while clinical teams focus on adherence trends and sentiment analysis. This flexibility ensures that stakeholders can zero in on the metrics most relevant to their goals, enabling them to adapt programs quickly to emerging trends.
Outcome Measurement
The dashboard tracks critical metrics for enterprise clients, such as new patient starts, average therapy duration, and adherence rates. Patients paired with mentors through PatientPartner stay on therapy an average of 133.5 days longer than those without mentor support. Additionally, 90% of patients paired with mentors report higher confidence in starting treatment. Companies using the platform have seen a 30% increase in treatment adoption and a 20% improvement in adherence within the first year. By connecting real-time data with immediate actions, the dashboard plays a key role in improving patient outcomes.
sbb-itb-8f61039
2. Virtual Telehealth Tracking (e.g., MAT Support)
Virtual telehealth tracking takes the centralized dashboard concept and applies it to medication-assisted treatment (MAT) programs. This approach enables real-time monitoring for patients in recovery, connecting them with mentors who have personal experience in similar challenges. By shifting peer mentorship from face-to-face interactions to digital platforms, these programs can now gather objective data on patient progress and engagement.
Real-Time Alerts
Digital platforms provide alerts that help mentors and care teams connect with patients during critical moments. Using tools like messaging and calls, they can reach individuals who might otherwise be inaccessible through traditional systems. These alerts aren't just functional - they bring a human touch to care, reminding patients that someone is actively supporting them through tough times. Paul Hoffman, CEO & Founder of inTandem Health, highlights this mission:
Our mission is to... insert a peer mentor onto the patient's care team, empowering new patients to face life-changing health challenges with a patient who has walked in their shoes.
Data Accuracy
One of the standout benefits of virtual telehealth tracking is the shift from self-reported updates to objective digital logs. This eliminates recency bias, offering more reliable data for decision-making. Accurate information is crucial for understanding adverse events and addressing patient concerns. With this level of precision, mentors can provide better situational analysis and design measures to reduce risks. In virtual settings like phone or video calls, having trustworthy data ensures that professional development and patient safety remain priorities.
Personalization
Real-time tracking also enables programs to tailor support based on each patient's risk score, which is updated continuously as new data comes in. Platforms conduct ongoing needs assessments, flagging additional support requirements as they arise. This allows mentors to focus their time and resources where they're needed most, moving away from a generic, one-size-fits-all approach.
Outcome Measurement
By combining accurate data and personalized support, virtual MAT programs can focus on tracking retention-in-treatment (RiT) as a key performance indicator. For instance, Bicycle Health achieved an impressive 80% retention rate at 90 days through virtual MAT and real-time support between 2022 and 2023 [doc]. This emphasis on adherence not only enhances value-based care but also reduces the likelihood of readmissions. Patrick Hays, Board Advisor at inTandem Health, underscores the value of this approach:
By introducing peer-to-peer mentor support in pre-service, you're helping health systems deliver value-driven healthcare while also reducing their risk.
3. Peer-to-Peer Remote Coaching (e.g., Diabetes Mentoring)
Peer-to-peer remote coaching takes telehealth a step further by combining real-time medical device data with personalized, condition-specific mentoring. For chronic conditions like diabetes, this approach connects patients with mentors who have firsthand experience managing the same condition. It’s more than just regular check-ins - mentors use real-time health data to provide timely, actionable support tailored to the patient’s needs. This creates a system where guidance is not only empathetic but also immediate and practical.
Real-Time Alerts
One of the standout features of these programs is real-time alerts. For example, if a patient’s blood glucose levels fall outside their target range, their mentor gets notified right away. This allows mentors to step in and provide guidance at critical moments, rather than waiting for scheduled check-ins. With data from Continuous Glucose Monitors (CGMs) feeding directly into coaching platforms, mentors can respond instantly, turning what used to be occasional advice into continuous, real-time support.
Data Accuracy
The integration of medical devices like CGMs and insulin pumps ensures that mentors have access to accurate, up-to-the-minute data. These devices generate a constant stream of information, giving mentors a clear picture of the patient’s daily patterns. This level of accuracy helps mentors offer advice that’s grounded in facts, not guesswork.
Personalization
With access to real-time data, mentors can provide advice that’s tailored to the patient’s specific circumstances. Coaching platforms also match patients with mentors who share similar experiences - such as the same type of diabetes, age group, or familiarity with devices like insulin pumps. This targeted approach ensures that the advice is not just relevant but also relatable. For instance, if a mentor notices a post-meal glucose spike in the patient’s data, they can draw on their own experience to offer practical, situation-specific tips. This shifts the focus from generic guidance to solving real problems in real time.
Outcome Measurement
To gauge the mentorship’s impact on patient decision making, platforms track key metrics like severe hypoglycemia or hyperglycemia incidents. Mentors are encouraged to maintain regular communication with their mentees, and the collected data is analyzed to evaluate how effective their strategies are. This focus on measurable outcomes helps refine the program, ensuring that the care provided remains timely, effective, and responsive to patient needs.
4. Healthcare Mentoring Platforms
Healthcare mentoring platforms take real-time tracking and apply it to patient support, offering a blend of technology and human connection. These platforms, similar to tools like the PatientPartner dashboard, combine immediate updates, precise data collection, tailored experiences, and progress tracking to guide patients through their treatment. They also simplify the challenge of pairing patients with mentors, monitoring their interactions, and evaluating the program's effectiveness - all in real time.
Real-Time Alerts
These platforms send instant notifications to coordinators when issues arise, such as missed sessions or concerning symptoms. This allows teams to step in quickly, addressing problems before they escalate.
Data Accuracy
By logging details like session length, discussion topics, and patient concerns as they happen, these platforms reduce the risk of memory-related errors. This ensures a more accurate understanding of mentorship dynamics and the obstacles patients encounter.
Personalization
AI-driven algorithms match patients with mentors based on shared experiences, treatment methods, and personal preferences. Unlike simpler tracking tools, these platforms manage large-scale mentorship programs with ease. They also monitor engagement in real time, making it easier to adjust pairings if needed. Research shows that mentoring programs can increase representation of underrepresented groups by 9% to 24%, and mentees are 98% more likely to recommend their organization as a great place to work.
Outcome Measurement
Real-time dashboards allow organizations to monitor key metrics like participation rates, session completions, and long-term retention. By setting baselines and aligning activities with SMART goals, these platforms provide a clear picture of progress and return on investment. This holistic view highlights their role in driving lasting, positive results.
Advantages and Disadvantages
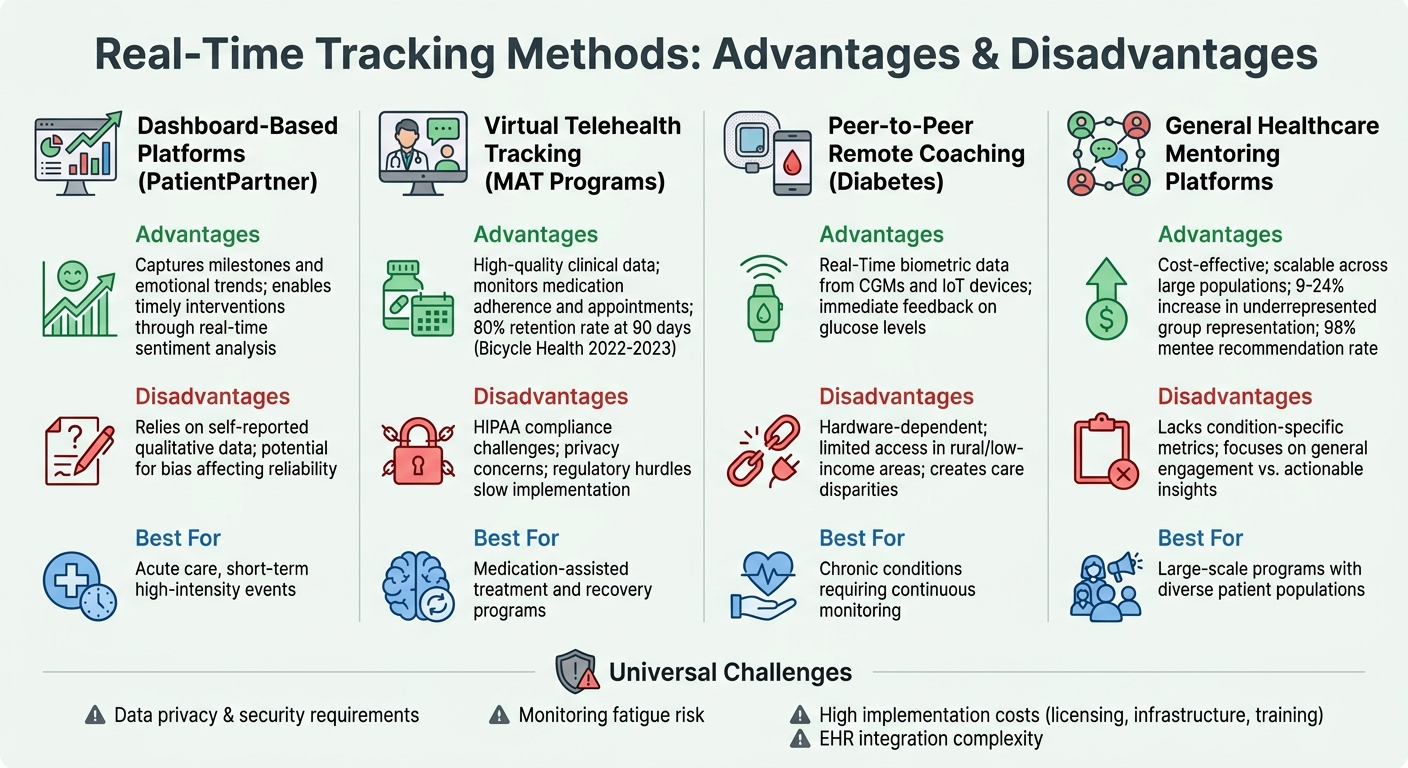
Comparison of Real-Time Tracking Methods in Patient Mentorship Programs
When it comes to real-time tracking in patient mentorship programs, each approach has its strengths and weaknesses. These systems have the potential to transform how mentors and patients interact, but they come with trade-offs that organizations must carefully consider.
Dashboard-based platforms, such as PatientPartner, shine in capturing milestones and analyzing emotional trends in peer-to-peer connections. These tools allow coordinators to detect emotional shifts as they occur, offering opportunities for timely interventions. However, they rely heavily on self-reported, qualitative data, which can introduce bias and affect the reliability of insights.
Virtual telehealth tracking is particularly effective in medication-assisted treatment (MAT) programs, where it provides high-quality clinical data by monitoring medication adherence and appointment attendance. The downside? Regulatory hurdles like HIPAA compliance and privacy concerns around recovery status can complicate implementation. These challenges may slow down mentor-patient interactions, making it harder to maintain a seamless experience.
For conditions like diabetes, peer-to-peer remote coaching integrates directly with tools like continuous glucose monitors (CGMs) and IoT devices, delivering real-time biometric data. While this approach ensures timely feedback, its reliance on specific hardware can limit access for patients in rural or low-income areas, creating disparities in care.
On the other hand, general healthcare mentoring platforms are cost-effective and can scale across large patient populations. However, they often lack the ability to track condition-specific metrics, focusing instead on general engagement data rather than actionable insights tied to specific diseases.
Data privacy and security remain a top priority across all tracking methods. Real-time transmission of sensitive health data demands robust measures, like end-to-end encryption and regular SOC2 Type II audits. Many platforms operate in isolated silos, complicating integration with a patient’s primary electronic health record (EHR). Using HL7 FHIR APIs can help resolve these interoperability issues, allowing mentorship data to flow into clinical workflows seamlessly.
Another challenge is monitoring fatigue. Patients may feel over-surveilled, which could reduce long-term participation. The best platforms address this by being transparent about what data is tracked and who can access it. They also allow administrators to customize tracking features based on the sensitivity of the medical condition, such as stricter controls for mental health programs compared to physical therapy.
Balancing proactive intervention with patient comfort is key. Real-time tracking eliminates recall bias and enables mentors to act during critical moments - like when a patient misses a dose or shows signs of distress. However, the costs of implementation, including licensing, infrastructure, training, and maintenance, can be high. Organizations need to weigh whether the benefits of continuous monitoring justify these expenses or if periodic check-ins are sufficient for lower-risk groups.
Ultimately, these trade-offs highlight the considerations needed to optimize patient mentorship programs while ensuring they remain effective and patient-focused.
Conclusion
Real-time tracking has shifted patient mentorship from occasional check-ins to proactive, data-informed support. While no single model works perfectly in every situation, each approach thrives in specific scenarios, depending on the treatment timeline and the level of clinical attention required.
Take PatientPartner as an example. Its dashboard is particularly effective for acute care, excelling in short-term, high-intensity events. By aligning mentorship with defined clinical timelines - like a 90-day recovery period - it helps improve patient readiness and encourages the adoption of new treatments. This approach is especially beneficial for pharmaceutical and med-tech companies aiming to increase patient starts and promote new therapies.
For chronic care, digital coaching platforms take things further. Peer-to-peer remote coaching, combined with automated wearable integration, removes the need for manual updates and provides real-time, accurate feedback. Similarly, telehealth-based Medication-Assisted Treatment (MAT) support enhances recovery by monitoring compliance and identifying early signs of relapse.
Choosing the right mentorship platform is essential. Look for systems that offer shared dashboards for patients, mentors, and providers, along with clear escalation protocols for handling deviations. The best platforms strike a balance between continuous monitoring and maintaining patient comfort.
Whether it’s acute milestone tracking, biometric syncing, or compliance monitoring, tailoring real-time tracking to the specific needs of patients leads to better outcomes.
FAQs
What data should we track in real time for a mentorship program?
Real-time mentorship programs, such as those offered by PatientPartner, thrive on tracking critical data to enhance both engagement and results. Key areas to monitor include patient adherence - this could mean tracking medication usage or ensuring patients attend their appointments. Another focus is mentor-patient interaction metrics, like how often they communicate, the length of those interactions, and how quickly mentors respond.
Additionally, keeping an eye on condition-specific health indicators is crucial. For example, monitoring blood sugar levels for diabetic patients can provide valuable insights. Incorporating sentiment analysis into these interactions allows mentors to better understand patients’ emotional states, enabling them to offer more personalized support. This approach not only strengthens patient adherence but also contributes to better health outcomes overall.
How do we prevent alert fatigue for care teams and mentors?
To avoid alert fatigue, it's crucial to focus on relevance and prioritization when managing notifications. Tailor alert settings to ensure that only critical or actionable notifications are sent. Leveraging smart algorithms can help filter alerts based on urgency or the level of patient risk, making them more manageable.
Additionally, establish clear communication protocols to streamline how alerts are handled. Make it a habit to review alert parameters regularly and adjust them based on team feedback. These approaches not only keep care teams and mentors engaged but also minimize unnecessary interruptions, allowing for more effective support without overwhelming anyone involved.
How can we keep real-time mentorship tracking HIPAA-compliant?
To maintain HIPAA compliance in real-time mentorship tracking, it's crucial to implement measures that safeguard patient privacy and secure health information. Start by using encryption to protect data during transmission and storage. Additionally, establish robust access controls to ensure only authorized personnel can view sensitive information.
Incorporating audit trails is another essential step. These logs help monitor access and activity, making it easier to detect and address any unauthorized actions. Always rely on HIPAA-compliant tools specifically designed for managing healthcare data, as they align with the necessary security standards.
Finally, limit access strictly to authorized individuals. This minimizes the risk of data breaches or unauthorized access, ensuring patient information remains protected.




