Q&A: Cultural Sensitivity in Patient Mentorship Programs

Key Takeaways
Understanding cultural differences in patient mentorship programs leads to better care and outcomes. When mentors acknowledge their biases and adapt to the needs of diverse patients, it builds trust and improves treatment adherence.
Key insights:
- Patients paired with relatable mentors are 68% more likely to start prescribed treatments and stay on therapy 133.5 days longer.
- Training mentors to recognize biases and use models like LEARN enhances their ability to connect with mentees.
- Feedback systems and tools like the Implicit Association Test help mentors refine their approach.
- Programs that respect patients’ traditions, beliefs, and decision-making processes see higher satisfaction and engagement.
The article highlights strategies to match patients with compatible mentors, train mentors effectively, and address systemic barriers to improve healthcare equity. These efforts result in better patient activation, attendance rates, and long-term health outcomes.
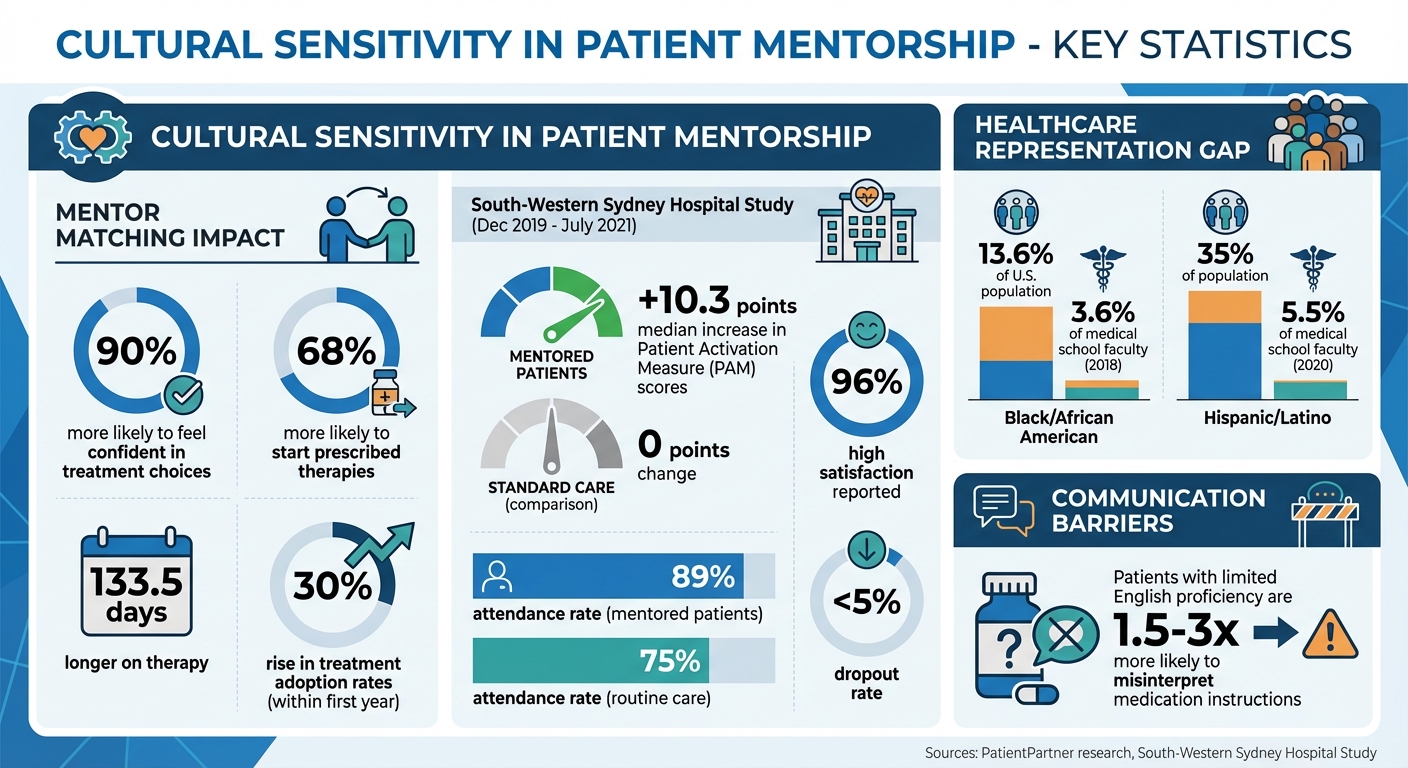
Impact of Cultural Sensitivity in Patient Mentorship Programs: Key Statistics and Outcomes
Bridging Difference: Building Cultural Competency in Mentoring with Lisa Fain
sbb-itb-8f61039
How Cultural Sensitivity Supports Patient-Centered Healthcare
Patient-centered care focuses on honoring each individual's preferences, needs, and values in every clinical decision. A key part of this is cultural sensitivity, which acknowledges that a patient’s background - like their traditions, beliefs, language, and family dynamics - shapes their healthcare experience. When mentorship programs embrace cultural awareness, they can provide care that respects and aligns with each patient’s identity. This approach refines mentorship strategies and patient support programs to better serve a wide range of needs.
This shift moves mentorship from a one-size-fits-all model to one that offers personalized support for diverse populations. Culturally aware mentors can address issues such as bias, microaggressions, and spirituality, while also understanding when to involve family members in cultures that value collective decision-making. For instance, Hispanic patients may benefit from having extended family included in treatment discussions, whereas LGBTQ+ patients might need mentors who understand the specific barriers they face in accessing healthcare.
These efforts have a direct impact on patient outcomes. Culturally sensitive mentorship fosters trust, helping to break down barriers like mistrust and miscommunication. When patients feel their cultural identity is acknowledged and respected, they are more likely to engage with their care. This leads to higher satisfaction, better adherence to treatment plans, and improved long-term health outcomes - particularly for groups that have historically faced systemic healthcare inequities.
Cultural sensitivity doesn’t just complement patient-centered care - it brings it to life. By addressing the diverse realities of patients’ lives, mentorship programs create relationships built on respect and trust. This connection empowers patients, turning uncertainty into active participation in their own healthcare journey.
Strategies for Building Cultural Sensitivity in Mentorship Programs
Approaches that prioritize cultural sensitivity can significantly improve patient engagement and treatment outcomes. A mentorship program that values cultural understanding creates relationships built on trust and respect for individual experiences. This kind of relationship goes beyond surface-level guidance, fostering meaningful connections that address patients' unique needs.
Matching Patients with Compatible Mentors
The starting point for culturally sensitive mentorship is finding common ground. When patients are paired with mentors who share similar cultural backgrounds or healthcare journeys, trust develops more naturally. Advanced patient engagement software makes it easier to identify mentors whose experiences resonate with patients. This kind of matching can alleviate fears and uncertainties that might otherwise deter patients from pursuing treatment.
PatientPartner employs automated systems to connect patients with mentors at the right time, ensuring interactions are both timely and secure under HIPAA compliance. The impact of this approach is clear: patients matched with relatable mentors are 90% more likely to feel confident in their treatment choices and 68% more likely to start their prescribed therapies. However, matching is only the first step - mentors also need to be prepared to navigate cultural differences effectively.
Training Mentors in Cultural Competency
Proper training is essential for mentors to engage meaningfully across cultural lines. Techniques like role-playing, case studies, and reflective journaling help mentors identify and address their own biases. One useful tool is the LEARN model, which guides mentors through steps to Listen, Explain, Acknowledge, Recommend, and Negotiate during their interactions.
A real-world example comes from a mentorship program implemented in three hospital-based clinics in Australia between December 2019 and July 2021. Here, six mentors with personal experience managing chronic pain supported patients from Arabic, Assyrian, and Vietnamese communities. These mentors underwent mandatory training and HR onboarding before starting their roles. The program led to a 10.3-point median increase in Patient Activation Measure scores, compared to no change in standard care. For programs seeking affordable training options, digital resources like the HHS "Think Cultural Health" courses offer accredited training modules lasting 4–5.5 hours.
Creating Feedback Systems for Continuous Improvement
Even with training, cultural sensitivity requires ongoing attention and refinement. Feedback mechanisms are crucial for maintaining high standards and adapting to new challenges. Automated systems can monitor mentor-patient interactions in real time, identifying areas for improvement while safeguarding privacy.
These systems provide immediate insights, enabling quick adjustments instead of waiting weeks for survey results. By aligning feedback with measurable outcomes - such as therapy initiation rates or treatment adherence - mentorship programs can demonstrate the tangible benefits of cultural sensitivity. For example, companies using mentor-driven platforms have reported a 30% rise in treatment adoption rates within the first year.
Common Barriers to Cultural Sensitivity in Patient Mentorship
Even with well-designed mentor matching and training, certain obstacles persist. One major issue is unconscious bias, which can lead mentors to misinterpret cultural behaviors as noncompliance. For instance, studies reveal that Black and Hispanic patients often receive less pain medication and have limited access to surgical treatments due to implicit biases among healthcare providers. A mentor might similarly misjudge a patient's culturally or religiously motivated decisions - like a Jehovah's Witness declining a blood transfusion - as defiance, rather than recognizing these choices as deeply rooted in personal beliefs.
Another challenge arises when mentors, lacking proper training, rely on stereotypes instead of tailoring care to the individual. However, training programs that address issues like oppression and marginalization have proven effective in equipping mentors to better navigate career challenges and contribute to health equity.
Systemic inequalities in healthcare further complicate mentorship. Despite Black and African American individuals making up 13.6% of the U.S. population in 2018, they represented only 3.6% of medical school faculty. Similarly, while Hispanic and Latino individuals accounted for 35% of the population in 2020, they made up just 5.5% of faculty. This underrepresentation creates a limited pool of culturally diverse mentors and places an added burden, often referred to as the "minority tax", on those from underrepresented backgrounds. Additionally, a report by the Institute of Medicine found that racial and ethnic minority groups consistently receive lower-quality healthcare - even when insurance coverage is equivalent to that of White patients.
Organizations can address these barriers through targeted strategies. Tools like the Implicit Association Test (IAT) help mentors uncover hidden biases and identify areas for growth. Shifting the focus from memorizing cultural facts to adopting cultural humility - a mindset that emphasizes curiosity, openness, and lifelong learning - can also make a significant difference. As Providence Ready explains:
Cultural humility is a mindset that values curiosity, openness, and lifelong learning. This means approaching each patient as an individual, understanding that cultural norms may vary even within the same community, and avoiding assumptions.
Building meta-mentorship systems, where mentors support one another in addressing difficult conversations about race and identity, is another effective approach to overcoming systemic challenges.
How Cultural Sensitivity Affects Patient Outcomes
The influence of culturally sensitive mentorship is evident in measurable improvements in patient outcomes. Between December 2019 and July 2021, three hospital-based clinics in South-Western Sydney introduced a "natural helper" program aimed at supporting patients from Arabic, Assyrian, and Vietnamese communities. This initiative resulted in a 10.3-point increase in PAM (Patient Activation Measure) scores for mentored patients, compared to no change in those receiving routine care. Attendance rates also saw a boost, with mentored patients achieving an 89% attendance rate and 96% reporting high satisfaction, compared to 75% attendance under routine care. These results underscore the tangible benefits of culturally tailored mentorship.
Patient activation - defined as a patient’s knowledge, skills, and confidence in managing their health - is a key factor in achieving long-term treatment success. Dr. Bernadette Brady's research team highlighted how mentors with shared lived experiences help bridge communication gaps that could otherwise lead to misunderstandings of medication instructions or discharge plans. Patients with limited English proficiency are 1.5–3 times more likely to misinterpret such guidance, making this mentorship even more critical.
One of the mechanisms driving these improvements is "expectational priming." When mentors share a cultural background and similar health journeys with their mentees, they help set realistic expectations for treatment while fostering a sense of understanding and trust. As one mentee noted, shared backgrounds and life experiences create a deeper sense of relatability and understanding.
Culturally sensitive mentorship also taps into the collectivist values often found in migrant communities, where shared experiences and community support significantly influence healthcare decisions. This approach not only enhances satisfaction but is also linked to better physiological outcomes, such as improved blood pressure, HbA1c levels, and cholesterol readings. Additionally, it promotes high patient engagement, with dropout rates falling below 5%. By integrating collectivist support into healthcare, this model reinforces the importance of cultural alignment in fostering better outcomes.
For organizations looking to implement patient mentorship programs, these findings emphasize that cultural sensitivity isn’t just about avoiding missteps or meeting diversity goals. It’s a practical, results-driven strategy that improves patient engagement, boosts attendance rates, and supports long-term health management.
Moving Forward with Culturally Sensitive Mentorship Programs
Culturally sensitive mentorship programs go beyond simply having good intentions - they require a fundamental shift from focusing on cultural competence to embracing cultural humility. Instead of memorizing cultural facts, organizations should encourage mentors and staff to cultivate curiosity, maintain openness, and commit to lifelong learning. Research consistently shows that this approach leads to measurable improvements in care and outcomes.
By prioritizing cultural sensitivity, organizations can actively address systemic disparities and tackle long-standing healthcare inequities, as highlighted in prior studies.
"Cultural sensitivity is not just a box to check. It's a mindset, skill set, and a lifelong commitment to understanding, respect, and partnership." – Providence Ready
Turning this commitment into action requires practical strategies. Tools like the Implicit Association Test can encourage regular self-reflection, while interactive role-playing and simulated patient scenarios help mentors develop the communication skills needed to interpret non-verbal cues and collaborate effectively with interpreters. Organizations can also promote inclusivity by using multilingual signage, respecting individuals' preferred pronouns, and incorporating cultural practices into care plans. These steps lay a strong foundation for integrating technology-driven solutions.
Digital tools play a critical role in maintaining these practices over time. For example, PatientPartner's platform personalizes mentor-patient connections, ensuring mentors understand the unique perspectives of those they support. This approach helps pharmaceutical and med-tech companies build trust and engagement, which are crucial for encouraging long-term treatment adherence. When combined with ongoing training and consistent feedback, these tools make cultural sensitivity a sustainable practice, ultimately improving care and outcomes for diverse patient populations.




