Collaborative Frameworks for Med-Tech Patient Support

Key Takeaways
In med-tech, connecting patients with the right support is a challenge. Collaborative frameworks help bridge the gap between advanced treatments and patient care. This article outlines four key frameworks that improve patient outcomes, streamline workflows, and integrate new technologies:
- Hierarchical Telemedicine Consortium Framework: Uses a tiered system and real-time data sharing to reduce treatment delays and improve care coordination.
- Collaborative Space-Analysis Framework (CS-AF): Promotes teamwork across organizations using shared platforms for remote monitoring and patient engagement.
- Service-Oriented Architecture (SOA) Collaboration Framework: Automates administrative tasks, enhancing efficiency and scaling med-tech programs.
- Role-Based Physician-Patient Collaboration Framework: Assigns specific roles to care teams and patients, improving adherence and resource use.
Each framework has its strengths and trade-offs, making the choice dependent on goals like reducing lead times, improving adherence, or scaling operations. By aligning frameworks with specific needs, med-tech companies can deliver better patient care while integrating advanced tools effectively.
Collaborative Care Models in Personalized Medicine (14 Minutes)
sbb-itb-8f61039
1. Hierarchical Telemedicine Consortium Framework
The Hierarchical Telemedicine Consortium Framework creates a structured system for patient care, guiding individuals from primary facilities to specialized centers based on their needs. It uses a two-way referral system to ensure patients are directed to the appropriate level of care depending on the severity of their condition. Central to this framework is the use of 5G-powered technology, enabling real-time data sharing and faster communication. A great example of this in action is the Henan Telemedicine Center (HNTC) at the First Affiliated Hospital of Zhengzhou University, which extends high-quality medical services to rural and primary hospitals through this well-organized approach.
Treatment Lead Time Reduction
This framework significantly cuts down on waiting times by aligning physician availability with patient demand through advanced scheduling. It also relies on unified data collection standards, which allow medical records and diagnostic information to flow seamlessly across different levels of the consortium. This eliminates delays caused by disconnected information systems, ensuring patients receive timely care.
"The optimal mechanism-integrated model outperforms the current fixed price model from the perspective of treatment costs for patients in the telemedicine center and the total cost of patient referral."
Scalability for Med-Tech Integration
The framework doesn’t just reduce delays - it also supports the integration of new medical technologies. Its ability to scale depends on the clinical context, with high-severity patients benefiting the most from telemedicine-enabled rapid response services. However, it works best when it streamlines care processes rather than adding unnecessary complexity. Med-tech companies are encouraged to focus on creating unified information platforms and using operations research to optimize how resources are allocated within the consortium.
2. Collaborative Space-Analysis Framework (CS-AF)
The Collaborative Space-Analysis Framework (CS-AF) takes a different path compared to the more rigid, tiered structure of the Hierarchical Telemedicine Consortium Framework. Instead of strict layers, it promotes adaptable, cross-organizational teamwork. By creating shared learning platforms, this framework allows independent health systems to swap strategies and tackle mutual challenges. It has already shown its value in national initiatives for electronic patient-reported outcomes (ePRO) and remote symptom monitoring. This approach doesn’t just enhance collaboration - it also helps improve patient adherence, as explored below.
Patient Adherence Rates
Boosting adherence in remote monitoring hinges on two key factors: clear communication of benefits and consistent feedback. The CS-AF incorporates feedback loops to quickly spot and address patient drop-offs, ensuring they stay engaged throughout their treatment. Transparent communication encourages patients to enroll, while ongoing monitoring and support from care teams help them stick with the program from start to finish.
Scalability for Med-Tech Integration
The framework’s adaptable structure makes it easier to roll out new technologies in a targeted way. Each organization can smoothly integrate new med-tech tools into their existing workflows. By working together on these shared platforms, organizations can tackle implementation challenges as a group, simplifying how patient monitoring technologies are adopted across various clinical settings.
3. Service-Oriented Architecture (SOA) Collaboration Framework
The Service-Oriented Architecture (SOA) Collaboration Framework takes a modular and automated approach to streamline mentorship operations. Instead of relying solely on rigid structures or shared platforms, it uses integrated tools and automation to manage resources effectively, especially within med-tech patient support programs. This setup minimizes manual tasks and ensures resources are allocated efficiently.
Resource Utilization
One of the key strengths of SOA-based frameworks is their ability to automate administrative processes that often burden program coordinators. Tasks like implementation and mentor-mentee matching are handled by automated platforms, freeing staff to focus on more strategic responsibilities. With the help of AI, mentors are matched to mentees based on specific needs, enhancing time management and overall program efficiency.
A great example of this efficiency comes from Barts Health NHS Trust. In April 2024, their Healthcare Horizons program used a mentoring platform provided by PLD Mentoring to assist young people in East London interested in healthcare careers. The platform’s intuitive design and robust reporting tools helped 75% of registered mentees successfully connect with mentors for career guidance, including support with UCAS applications and university interviews.
"The platform is very user-friendly for both end users and administrators and has many features and useful reporting dashboards. This allows the organisation to report on the uptake, usage and satisfaction with programmes via evaluation surveys."
- An Organisation Development Business Partner at East London NHS Foundation Trust
The framework also offers real-time dashboards that provide insights into program uptake, usage, and satisfaction. This centralized visibility helps organizations direct resources toward active mentorship pairs while avoiding wasted effort on inactive connections. Predictable software costs make it easier for organizations to budget while scaling their services.
This level of efficiency is key to supporting broader med-tech integrations.
Scalability for Med-Tech Integration
The SOA framework’s operational efficiency makes it ideal for scaling med-tech initiatives. For instance, the OncoPRO initiative (Oncology Patient-Reported Outcomes Remote Symptom Monitoring Initiative) demonstrated the scalability of SOA principles from March 2023 to December 2024. Backed by PCORI, this national learning collaborative helped 12 independent health systems adopt electronic patient-reported outcomes (ePRO) and remote symptom monitoring. Through the initiative, researchers tackled 29 barriers and implemented 37 strategies across six domains, such as technical support and shared learning frameworks, to drive the adoption of complex oncology interventions.
"As the initiative matured, strategies targeting specific barriers (e.g. develop and implement quality monitoring systems) were added to support site-level operationalization and continuous improvement."
- Nicole Lynn Henderson, lead author from the University of Alabama at Birmingham
This modular framework enables seamless integration of new med-tech tools into existing workflows. By addressing challenges like clinician buy-in and technical compatibility, the framework supports expansion across different organizational environments and IT systems.
4. Role-Based Physician-Patient Collaboration Framework
The Role-Based Physician-Patient Collaboration Framework establishes a structured model where healthcare providers and patients take on specific roles throughout the treatment process. Physicians, nurses, care coordinators, and patients are each given distinct responsibilities to promote better communication and create an organized support system. Though research on this framework is still developing, it aims to improve patient involvement, streamline resource use, and support growth in healthcare systems.
Patient Adherence Rates
By clearly defining roles, this framework helps patients understand their responsibilities - like tracking symptoms, sharing health updates, or attending follow-up visits - making it easier to stick to their care plans. Platforms such as PatientPartner fit into this model by connecting patients with experienced mentors who guide them through their healthcare journey. These mentors work alongside clinical teams, offering practical support and helping patients use digital health tools effectively, complementing the guidance provided by healthcare professionals.
Resource Utilization
With roles clearly assigned, care teams can work more efficiently. Clinicians focus on medical decisions, coordinators handle logistics, and mentors provide daily support. This division of labor allows med-tech companies to better allocate resources, offering training and support tailored to each role. It also ensures that new digital tools or therapies are introduced in a way that aligns with the team’s specific responsibilities.
Scalability for Med-Tech Integration
A role-based framework makes it easier to expand patient support programs. Standardized roles allow organizations to replicate successful strategies by training new team members on well-defined responsibilities. This approach is especially valuable for pharmaceutical and med-tech companies launching therapies that require extensive patient education and ongoing monitoring. Assigning ownership for tools like remote monitoring devices or patient-reported outcome systems ensures consistent and effective implementation, helping teams deliver reliable support over time.
Advantages and Disadvantages
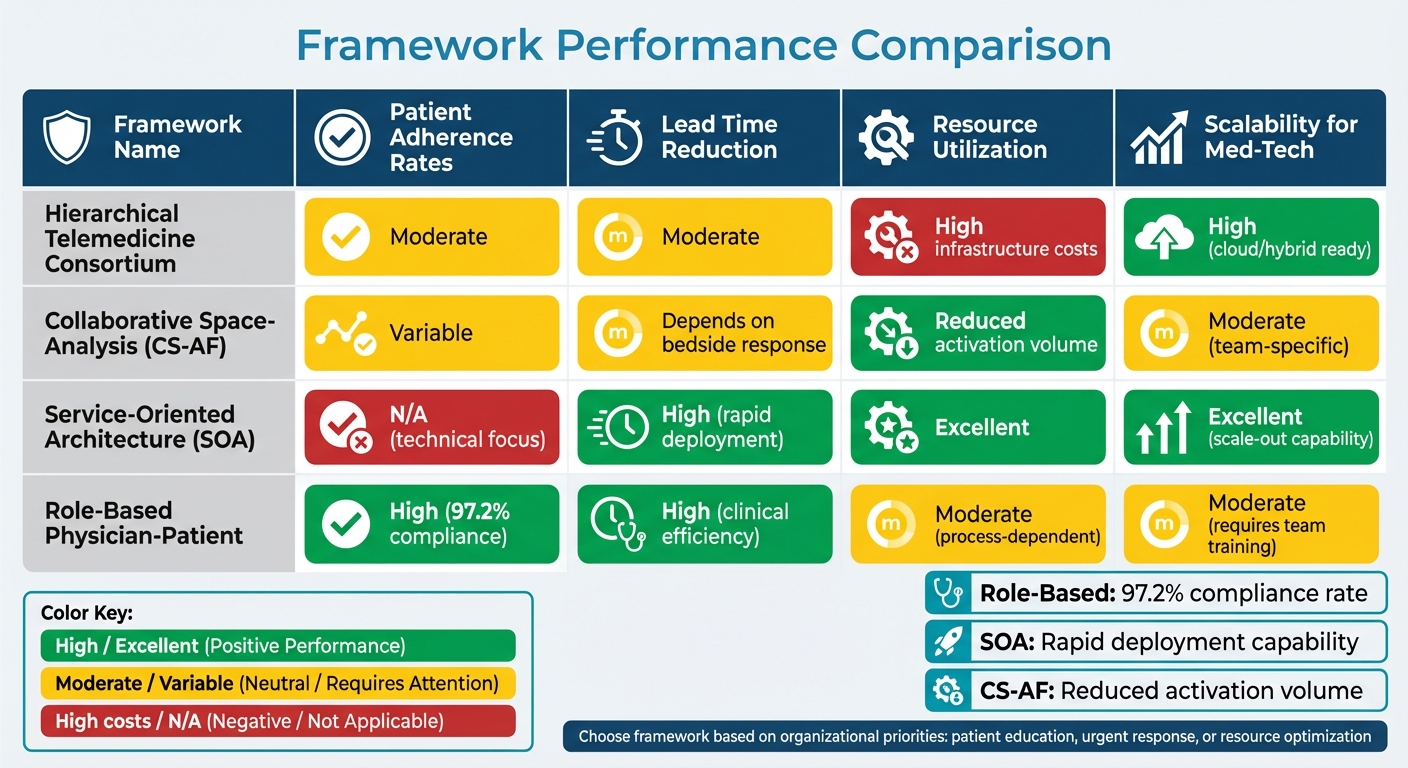
Comparison of Four Med-Tech Patient Support Frameworks: Performance Metrics
When it comes to patient support programs in med-tech, each framework has its own set of strengths and limitations. Understanding these trade-offs is crucial for selecting the right approach.
Take automatic escalation models, for example - they drastically cut team activation time from 25 to 7 minutes and door-to-balloon time from 125 to 86 minutes. However, this speed can lead to an uptick in rapid response calls, which might overburden clinical teams. On the other hand, bedside discretion models reduce unnecessary activations (13 calls versus 18 calls per ~1,900 patients), but they may delay critical interventions when time is of the essence.
Resource usage also varies significantly. Service-Oriented Architecture (SOA) frameworks stand out for their energy and space efficiency, making them ideal for scaling med-tech operations. Role-based frameworks, meanwhile, improve prescribing accuracy to 97.2%, up from 58.9%, but they require continuous team training to maintain these results. Hierarchical telemedicine consortiums ensure high system availability but come with hefty upfront infrastructure costs.
Another challenge is the "readmission paradox." For instance, telemedicine collaboration has been shown to cut hospital stays by 1.03 days and save $2,011.05 per acute kidney injury patient. Yet, it also increases the risk of readmission by 18%. Addressing this issue may require post-discharge strategies, such as patient mentorship, to ensure long-term adherence and success.
Here’s a quick comparison of these frameworks based on key performance metrics:
| Framework | Patient Adherence Rates | Lead Time Reduction | Resource Utilization | Scalability for Med-Tech |
|---|---|---|---|---|
| Hierarchical Telemedicine Consortium | Moderate | Moderate | High infrastructure costs | High (cloud/hybrid ready) |
| Collaborative Space-Analysis (CS-AF) | Variable | Depends on bedside response | Reduced activation volume | Moderate (team-specific) |
| Service-Oriented Architecture (SOA) | N/A (technical focus) | High (rapid deployment) | Excellent | Excellent (scale-out capability) |
| Role-Based Physician-Patient | High (97.2% compliance) | High (clinical efficiency) | Moderate (process-dependent) | Moderate (requires team training) |
Choosing the right framework depends on your priorities. If patient education is a focus, role-based models are a strong option. For urgent responses, automatic escalation is a better fit, while bedside discretion works well for optimizing resources. Incorporating patient mentorship into any framework can help tackle long-term challenges like adherence and readmissions.
Conclusion
Choose a framework that aligns with your goals and operational needs. For patient mentorship, the 6 C's framework - Connect, Communicate, Collaborate, Circulate, Cultivate, Celebrate - stands out as an effective option for large-scale programs. This model not only drives measurable results but also keeps participants engaged. For example, over 80% of participants remain active after being matched when given clear starting points, and 98% rate their mentoring experience as helpful when structured conversation frameworks are in place.
The key to success lies in pairing this framework with a strong support system. As Chronus highlights, “Mentoring programs can fail when participants simply don’t know where to start”. Structured guidance eliminates uncertainty, with 82% of participants describing their sessions as "very helpful" or even a "breakthrough" when using conversation prompts.
PatientPartner integrates the 6 C's framework with real-time mentorship technology to connect patients with experienced mentors. This combination supports long-term adherence and improves outcomes.
FAQs
Which framework fits my patient support goal?
When it comes to choosing the right framework, it all boils down to your goals. If your focus is on boosting patient adherence and engagement through tailored, real-time guidance, a mentorship framework could be the way to go. This approach builds strong relationships, encourages better outcomes, and improves adherence.
On the other hand, if scalability and structured support are your top priorities, a collaborative framework might be a better fit. With shared communication and integrated systems, this model streamlines processes and ensures efficient support. Ultimately, the framework you select should align with your mission to enhance patient engagement and outcomes.
What data and IT setup do these frameworks require?
To effectively manage real-time patient engagement data, these frameworks need strong digital platforms. Key elements include integration with electronic health records (EHRs), ensuring systems are secure and HIPAA-compliant, and leveraging cloud-based solutions to handle growth and scalability. Additionally, they depend on tools designed for tracking medication adherence, monitoring health metrics, and analyzing engagement activity. Secure communication channels and advanced analytics play a vital role in monitoring progress and tailoring support to individual needs.
How can mentorship reduce drop-offs and readmissions?
Mentorship plays a key role in reducing patient drop-offs and readmissions by building trust, enhancing understanding of medical conditions and treatments, and promoting adherence to care plans. Through structured mentoring, patients receive consistent guidance, which helps address concerns early and reinforces healthy habits. This kind of support keeps patients engaged, informed, and motivated, ultimately leading to improved health outcomes and a reduced need for further hospital visits or interruptions in treatment.




