Mentorship Guidelines for Pharma and Med-Tech Teams

Key Takeaways
Mentorship programs in pharma and med-tech are essential for bridging the gap between leadership goals and frontline execution. These programs help align team efforts, improve patient care, and ensure compliance with complex regulations. Here’s what you need to know:
- Why Mentorship Matters: Builds trust among clinicians, improves team collaboration, and supports patient-centered care by connecting experienced professionals with newer team members.
- Key Benefits: Enhances patient adherence, simplifies regulatory navigation, and aligns product development with patient needs.
- How to Succeed: Set clear goals using SMART objectives, track progress with measurable KPIs, and ensure mentor-mentee matches are well-aligned based on skills and goals.
- Technology's Role: Virtual platforms expand access to mentorship, enabling global connections and real-time support.
- Compliance and Ethics: Adhere to regulations like HIPAA, the Anti-Kickback Statute, and the Sunshine Act to maintain program integrity.
Mentorship is a strategic tool for improving patient outcomes, fostering team growth, and navigating the challenges of the healthcare industry effectively.
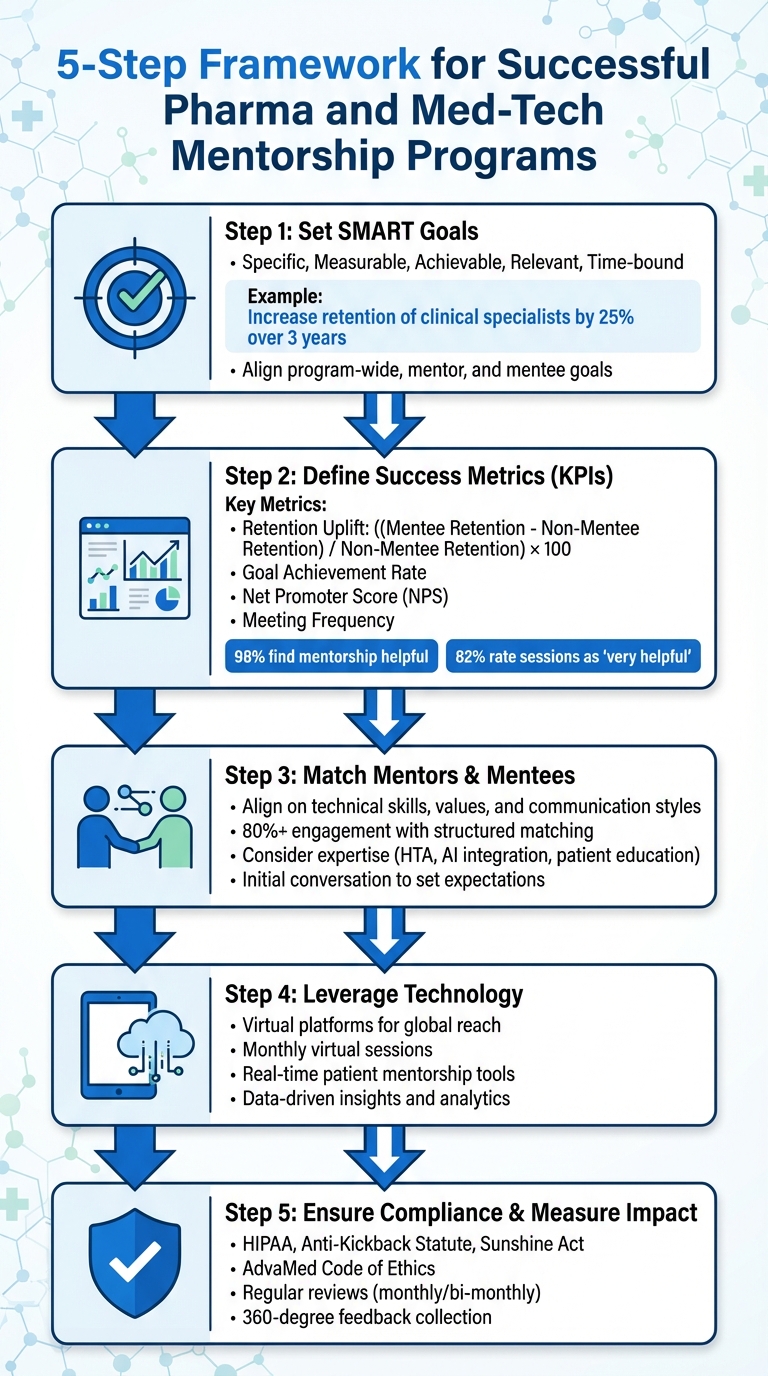
5-Step Framework for Successful Pharma and Med-Tech Mentorship Programs
JHU Biotech/Pharma Industry Mentor Match Program
sbb-itb-8f61039
Setting Goals and Objectives for Mentorship Programs
Clear goals turn mentorship into a tool that delivers measurable results. Without specific targets, mentorship programs can lose focus and fail to deliver value. Using SMART objectives - Specific, Measurable, Achievable, Relevant, and Time-bound - provides a framework for tracking progress and proving success. For instance, instead of setting a vague goal like "improve team performance", a SMART objective could be: "increase retention of clinical specialists by 25% over three years".
Aligning goals at every level - program-wide, mentor-specific, and mentee-focused - is key to achieving meaningful outcomes. Take the example of a pharmaceutical company launching a mentorship program to develop future leaders. Mentors might focus on honing their coaching abilities, while mentees aim for promotions. Both goals align with the company’s broader mission, while giving each participant a clear personal incentive.
As discussed earlier, clinician feedback plays a role here too. Setting clear goals helps teams prepare for patient-centered care. Establishing baseline metrics, like a 70% retention rate, provides a way to measure progress. Matthew Reeves, CEO of Together Mentoring, highlights this multi-level approach:
A successful mentorship program requires managing goals on three levels at once - program administrator goals, mentor goals, and mentee goals. Aligning all three is what drives real results.
Connecting Mentorship Goals to Patient Engagement
Mentorship goals should directly support better patient outcomes. Mentoring enhances communication skills, helping teams explain treatments clearly and improve patient adherence. For example, setting goals like reducing the time it takes for strategies for enhancing patient engagement to reach full productivity or increasing patient satisfaction can connect mentorship efforts to broader healthcare priorities.
Tracking clinical skills is equally important. Mentors can guide mentees in applying theoretical knowledge to real patient scenarios. Imagine a pharmaceutical team working on a new diabetes medication. A practical goal might involve mentees conducting patient education sessions under mentor supervision. This hands-on experience builds confidence and ensures the team is ready to support patients once the medication is launched. Such alignment not only enhances team readiness but also sets the stage for tracking performance through clear KPIs.
Identifying KPIs to Measure Mentorship Performance
To evaluate mentorship effectiveness, focus on measurable metrics like program reach, mentee growth, mentor quality, engagement levels, and organizational ROI. These KPIs translate mentorship success into terms that resonate with leadership.
One key metric is the retention uplift percentage, calculated as:
((Retention Rate of Mentees - Retention Rate of Non-Mentees) / Retention Rate of Non-Mentees) x 100.
For example, if mentored employees have an 85% retention rate compared to 68% for non-mentored peers, this signals a strong impact. Other valuable KPIs include the Goal Achievement Rate (the percentage of mentees who meet their objectives), Meeting Frequency (ensuring regular mentor-mentee interactions), and the Net Promoter Score to assess overall satisfaction.
Pre- and post-program assessments can measure skill improvement, offering tangible proof of progress. Additional metrics, like tracking how quickly new hires reach full productivity with a mentor, monitoring mentee-to-mentor ratios to avoid burnout, and using pulse surveys to gauge confidence and mentor quality, provide early insights into program performance.
Data underscores the value of structured mentoring platforms: 98% of participants find the experience helpful, while 82% describe their sessions as "very helpful" or even a "breakthrough". With guided conversation frameworks, over 80% of participants remain engaged after being matched. These benchmarks not only help set realistic expectations but also signal when adjustments are needed to keep the program on track.
Matching Mentors and Mentees Effectively
The success of a mentorship often hinges on finding the right match. When mentors and mentees share core values, align in expertise, and communicate effectively, their collaboration thrives - and so do patient outcomes. In fact, studies reveal that over 80% of participants in structured mentorship programs remain engaged when thoughtful matching processes are in place. This process begins with a clear understanding of what both parties bring to the table. It's not just about seniority or availability; it’s about identifying the specific technical skills a mentee needs, such as proficiency in AI integration or value-based procurement. Starting with these deliberate criteria lays the groundwork for meaningful mentorships that address the unique challenges of the pharmaceutical and med-tech industries.
Selecting Qualified Mentors in Pharma and Med-Tech
The next step is choosing mentors who align with these well-defined criteria. Ideal mentors combine technical expertise with knowledge in areas like value-based procurement, health technology assessment (HTA), and supply chain transformation. But technical know-how alone isn’t enough. As Sir Walter Bodmer, FRS, aptly put it:
Learn to communicate with the public, be willing to do so and consider it your duty to do so.
This mindset is essential for mentors guiding teams toward patient-centered care.
The most effective mentors are approachable, analytical, and excellent listeners. They foster two-way conversations, moving away from the traditional "deficit model" of communication. These mentors also tackle ethical questions surrounding new technologies, assess competency frameworks like Entrustable Professional Activities (EPAs), and understand tools like patient-reported outcome measures (PROMs). By doing so, they contribute to responsible research and drive meaningful change in healthcare. This thoughtful approach ensures that mentorship not only supports professional development but also fosters better patient adherence and satisfaction.
Using Personalized Matching to Improve Results
Tailored matching processes are essential for building strong mentor-mentee relationships and improving patient outcomes. Shared values and compatible working styles create a vision that directly enhances patient care. Personalized matching considers factors like communication preferences, professional goals, and specific expertise - rather than just job titles or seniority. For example, a mentee aiming to improve patient adherence in a new diabetes treatment program might benefit more from a mentor experienced in patient education than from a high-ranking executive with a broader leadership focus.
Structured mentoring programs that use guided conversations and values-based pairing deliver impressive results: 82% of participants report their sessions as highly impactful, and 98% rate their overall experience positively. These programs help mentees gain fresh perspectives on clinical challenges, which is critical for addressing barriers to treatment adherence. As Kina Vyas and Rhianna Nathwani observed in The Pharmaceutical Journal:
Ultimately, this enhances patient care by helping the pharmacist see situations from another perspective.
Before finalizing a match, it’s helpful to have an initial conversation to set expectations, address any potential conflicts, and outline specific patient-care goals. This ensures both mentor and mentee are aligned and ready to collaborate effectively. By focusing on personalized matches, teams can better support patient-centered care and drive meaningful improvements in healthcare delivery.
Using Technology to Support Mentorship Programs
Digital platforms are breaking down barriers, making mentorship accessible regardless of location. They allow mentors from major industry hubs to connect with early-career researchers and professionals across the United States and Puerto Rico, creating opportunities that go beyond traditional, in-person programs. This approach provides a structured way to expand mentorship programs and reach a broader audience.
Implementing Virtual Mentorship for Broader Reach
Platforms like the SMDP Mentoring Portal are leading the charge by offering consistent, monthly virtual mentoring sessions. In 2026, the International Center for Professional Development (ICPD) is leveraging this tool to support its Biotech and MedTech career mentoring initiatives. Through the program, SMDP Scholars work with industry mentors from leading companies such as Johnson & Johnson, Amgen, and Eli Lilly. Over the course of a year, these mentor-mentee pairs collaborate on personalized, trackable plans, meeting virtually each month. This virtual model has proven effective in extending mentorship opportunities, while real-time platforms are further enhancing patient engagement.
How PatientPartner Enables Real-Time Mentorship
PatientPartner takes mentorship a step further by focusing directly on patients. The platform connects patients with mentors who have firsthand experience with similar treatments. This addresses a key challenge: many patients struggle with adherence not because they lack information, but because they need someone who can genuinely relate to their journey. By using virtual tools, pharma and med-tech teams can bridge the gap between treatment initiation and adherence.
For these teams, PatientPartner offers more than just connections - it provides actionable insights through data-driven patient sentiment analytics and a compliance-ready infrastructure that scales for enterprise clients. Its personalized mentor-matching system ensures patients receive support tailored to their treatment paths, whether they’re starting a new oncology medication or preparing for a joint replacement. By fostering these peer-to-peer relationships, PatientPartner helps drive new patient starts, improve adherence, and enhance outcomes. This approach transforms mentorship into a patient-focused care strategy with measurable benefits.
Maintaining Compliance and Ethical Standards
Pharma and med-tech mentorship programs operate in one of the most heavily regulated areas of healthcare. Strong compliance measures are essential to ensure these programs run both legally and ethically. For example, the AdvaMed Code of Ethics - updated in October 2025 - provides guidelines for consulting arrangements, training sessions, and educational interactions with Health Care Professionals. These measures create the ethical foundation necessary for mentorship programs to function effectively within such a structured environment.
Meeting Regulatory Requirements
Mentorship programs must align with various federal laws to remain compliant. The Anti-Kickback Statute (AKS) and Stark Law mandate that these programs avoid any suggestion of illegal compensation that could influence referrals or purchasing decisions. The Sunshine Act adds another layer by requiring that any transfer of value - such as travel reimbursements, meals, or honoraria provided to physician mentors - be accurately tracked and reported through the Open Payments system. Additionally, the False Claims Act applies when there’s improper billing or submission of inaccurate claims to government healthcare programs.
Mentorship programs must also adhere to promotional regulations set by the FDA and FTC, ensuring that discussions remain focused on scientific and educational topics rather than unauthorized marketing. To manage these complexities, regular risk assessments, clear Standard Operating Procedures (SOPs), and interactive training sessions are crucial. Programs like AdvaMed's specialized compliance training can be particularly helpful in maintaining adherence to these regulations.
Protecting Patient Privacy and Data
When mentorship activities involve patient information - whether in clinical training or patient-to-patient interactions - HIPAA compliance becomes critical. Privacy protocols are reinforced through online training modules that are concise yet comprehensive. All participants must complete mandatory HIPAA training before engaging in program activities, with annual updates and centralized tracking to ensure long-term compliance. Additionally, encryption of all devices used in the program is a must, following established data security standards. A dedicated Data Security Program should oversee compliance with both internal policies and federal laws, ensuring sensitive information remains protected.
Measuring Program Performance and Impact
Once goals are set and mentor-mentee connections are established, tracking performance becomes essential to ensure the program delivers meaningful results. As Matthew Reeves, CEO of Together, puts it: "If you can't measure it, you can't improve it". By focusing on the right data points, mentorship evolves from a helpful initiative into a strategic tool that drives measurable outcomes.
Choosing the Right Success Metrics
The key to effective measurement lies in selecting metrics that reflect program reach, mentee growth, mentor effectiveness, engagement, and overall impact on the organization. For example, you can measure skill development by comparing pre- and post-program competency scores using this formula:
((Post-Program Score - Pre-Program Score) / Pre-Program Score) x 100.
If a mentee's patient communication score improves from 60 to 78, that's a 30% increase.
Tracking goal achievement is another critical metric. Record the percentage of mentees who meet their objectives - whether it's improving patient adherence strategies, mastering new med-tech tools, or advancing clinical communication skills. Additionally, the Net Promoter Score (NPS), which subtracts the percentage of detractors from promoters, offers valuable insights into satisfaction levels. Logging mentoring session frequency can also provide a real-time view of relationship health, making it essential to document meetings in a shared system.
To assess organizational impact, compare retention rates between participants and non-participants. Calculate the return on investment (ROI) by multiplying the number of employees retained above the baseline by the average cost of replacing an employee. Another useful metric is the time it takes for new hires to reach full productivity - with and without mentorship. This comparison highlights the program's effectiveness in accelerating onboarding. Together, these metrics create a solid foundation for ongoing evaluation and improvement.
Scheduling Regular Reviews and Feedback Sessions
Gathering feedback at various stages - registration, after sessions, mid-program, and at the end - ensures the program stays on track. Program managers should review collected data monthly or bi-monthly to identify trends or address potential issues early. Automating post-session feedback requests can make this process seamless and consistent.
It's important to distinguish between regular monitoring throughout the program and a comprehensive evaluation at its conclusion. Incorporating 360-degree feedback from participants' direct managers adds depth, offering insights into observed growth and behavioral changes. Combining quantitative data, like session ratings, with qualitative feedback and video testimonials provides a well-rounded view of the program's impact. This approach directly connects mentorship’s impact on patient decision-making to improvements in areas like patient adherence and care quality.
For smaller programs (under 25 participants), spreadsheets may be sufficient for tracking. However, larger initiatives benefit from specialized software that automates data collection and provides clear, easy-to-read reports.
Conclusion
Mentorship programs in the pharma and med-tech industries play a crucial role in advancing professional growth while enhancing patient engagement. When designed thoughtfully, these programs help bridge the gap between what patients need and what is often assumed they need. As Natalie Yeadon points out:
In many cases, the opinions from their peers is considered as valuable as that of their doctor.
This peer-to-peer connection allows patients to take an active role in their healthcare journey.
To achieve meaningful outcomes, patient-centered care requires clear objectives, effective mentor-mentee pairing, strict adherence to protocols, and ongoing performance tracking. By focusing on metrics like skill development and goal completion, organizations can improve patient adherence, boost health literacy, and help patients understand how their actions - like taking medications or following treatment plans - impact their overall well-being.
Technology has made scaling mentorship programs easier than ever. Digital tools, such as an AI patient mentor, enable real-time, virtual engagement, offering flexibility and accessibility. For example, PatientPartner (https://patientpartner.com) connects patients with experienced mentors who guide them through their healthcare experiences. This platform not only supports new patient enrollments but also fosters long-term adherence and better health outcomes.
Engaged patients don't just benefit personally - they also contribute to measurable business growth. Companies that regularly assess and refine their mentorship initiatives through stakeholder research are better equipped to succeed. By embedding patient engagement into every phase of the product lifecycle [16, 17], pharma and med-tech organizations can create programs that deliver lasting value for both patients and businesses.
FAQs
How do we pick mentorship goals that tie to patient outcomes?
To make mentorship truly impactful, it's essential to focus on personalized support that directly contributes to better health outcomes. For example, mentorship programs can help patients improve medication adherence or achieve more consistent blood sugar control. By designing mentorship activities with specific, measurable health goals in mind, you create a clear link between mentoring efforts and tangible improvements in patient well-being.
What KPIs best prove mentorship ROI to leadership?
Key performance indicators (KPIs) that showcase the return on investment (ROI) of mentorship programs include:
- Participant satisfaction: Gauges how well the program meets the expectations and needs of mentors and mentees.
- Skill development: Tracks improvements in specific skills gained through mentorship.
- Goal achievement: Measures how effectively participants reach their personal and professional goals.
- Retention and promotion rates: Evaluates whether mentorship contributes to keeping employees and advancing their careers within the company.
- Program engagement levels: Assesses participation and involvement to ensure the program remains impactful.
These metrics provide a clear, measurable way to connect mentorship efforts to business results, giving leadership a solid foundation to evaluate its overall value.
How can we run mentorship programs while staying compliant?
To ensure your mentorship programs meet compliance standards, it's crucial to start with clear guidelines and a thorough understanding of industry regulations. Properly training mentors is key - this includes aligning them with both legal and ethical standards to avoid potential pitfalls.
When dealing with sensitive information, such as patient data, always use a secure, HIPAA-compliant platform. This not only protects privacy but also ensures you're adhering to regulatory requirements. Additionally, conducting regular audits and gathering feedback helps identify any risks and keeps the program operating within compliance standards.
Finally, setting measurable goals is a smart way to maintain accountability. This approach ensures that your program stays aligned with both its objectives and regulatory boundaries.




